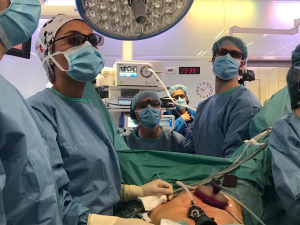
Transanal total mesorectal excision into the future
Last November in AIS Channel, we have celebrated the 10th anniversary of the first transanal total mesorectal excision (taTME) procedure (Figure 1). In that Thursday afternoon, we began by talking about the past, the road that led us to the first procedure, the important parts played by Patricia Sylla (1) and Richard Heald (2), and the present reality that we are facing in current days. During 7 and a half hours, in a record breaking eco-friendly event, fully created and fully transmitted on-line, with over 20,000 viewers, we discussed every single aspect of taTME.
Talking about the past is much easier than talking about the future and where we are heading to. Nevertheless, my role today is to do so.
I’m not going to try and see what the future beholds, that, I leave to crystal balls and magicians, but I’m going to give you my vision on what are the crucial steps to take taTME into the future: solid evidence and adequate proctoring.
Last year we had some important publications that have shaken the taTME-pro community. The Norwegian moratorium (3) took us by surprise, and has shown us that starting the taTME program could have serious implications. It led to disbelieve and discredit of a procedure that, until then, was thought to be effective and, at least, as oncologically safe as the other types of TME (open, laparoscopic, robotic).
It was not the first time we have witnessed something like it. The same thing happened in the 1990s with the fear of port-site metastases after oncologic resections (4) and the negative impact it had on laparoscopy. Later, it was proven that the technical aspects of the procedure were crucial in avoiding such complications and that they were an independent risk factor (5). As seen in that time, the scientific community promptly responded, showing their good results and questioning the data presented (6,7).
Just this January, a multicenter cohort study with 767 patients has proven that in high volume centers, taTME is associated with good locoregional control and that the technique, when adequately performed, does not imply an inherent oncological risk (8).
Although there is piling evidence in favor of taTME, I believe that only the results of the COLOR III trial (9) will close all the debates. This multicenter RCT is key in answering all the questions and clearing all the doubts regarding taTME’s role and, presumably, superiority in comparison with LapTME. The sooner we reach the numbers, the sooner we will have the results, so I ask all of you performing this technique, to submit your patients.
After 10 years, I have no doubt this procedure is the best way to treat mid and low rectal cancer and my hope is that it becomes consensual.
The other important issue that will influence the future of taTME is the way we train our surgeons to perform it—the proctoring. Ideally, a surgeon must have experience in TAMIS procedures and Laparoscopic colectomies before starting his training in taTME.
Published data shows that the better oncological results and the less contradictory conclusions come from centers of high volume, and, consequently, high expertise.
So, if we want to take this technique into the future, we must define what the ideal proctoring strategy is and how to evaluate the results of our trainees.
In our Hospital, since 2012, we have received more than 600 surgeons in the taTME hands-on course. Many of them currently perform the technique and are well known for their contributions, but others never came to implement it.
Critics say taTME is not for every surgeon, it has a very steep learning curve, it needs some very specific and expensive material and when performed with two teams, a bigger operating room and a higher number of personnel involved (Figure 2). I agree with the learning curve and the importance of overcoming difficulties before starting a program, but the only way to do it is to have an effective training.
As for everything, a way of someone learning something, may differ from the one beside him, and learning and training must be individualized. Our experience in online courses with our KHIRUS platform, with hands-on courses and, most recently, with telestration, made us re-think our proctorship of taTME. Starting this year, we will embrace a more comprehensive and personalized strategy, hoping to identify the ideal pathway for training surgeons in taTME and assure the continuity of this technique.
In conclusion, when we have the expected evidence on safety and oncologic results and when we master the proctoring pathway, we will lead taTME into the future and establish its role as the standard of care for mid and low rectal cancer.
Acknowledgments
Funding: None.
Footnote
Provenance and Peer Review: This article was commissioned by the Guest Editors (Satish Kumar Warrier and Alexander Heriot) for the series “taTME” published in Annals of Laparoscopic and Endoscopic Surgery. The article was reviewed by Dr. Satish Kumar Warrier and Dr. Alexander Heriot.
Conflicts of Interest: All authors have completed the ICMJE uniform disclosure form (available at http://dx.doi.org/10.21037/ales-2019-tatme-07). The series “taTME” was commissioned by the editorial office without any funding or sponsorship. AML serves as an unpaid editorial board member of Annals of Laparoscopic and Endoscopic Surgery from Mar 2017 to May 2021. FB de Lacy reports personal fees from Medtronic, personal fees from Olympus, personal fees from Applied Medical, personal fees from Conmed, outside the submitted work. The authors have no other conflicts of interest to declare.
Ethical Statement: The authors are accountable for all aspects of the work in ensuring that questions related to the accuracy or integrity of any part of the work are appropriately investigated and resolved.
Open Access Statement: This is an Open Access article distributed in accordance with the Creative Commons Attribution-NonCommercial-NoDerivs 4.0 International License (CC BY-NC-ND 4.0), which permits the non-commercial replication and distribution of the article with the strict proviso that no changes or edits are made and the original work is properly cited (including links to both the formal publication through the relevant DOI and the license). See: https://creativecommons.org/licenses/by-nc-nd/4.0/.
References
- Sylla P, Willingham FF, Sohn DK, et al. NOTES rectosigmoid resection using transanal endoscopic microsurgery (TEM) with transgastric endoscopic assistance: a pilot study in swine. J Gastrointest Surg 2008;12:1717-23. [Crossref] [PubMed]
- Heald RJ, Husband EM, Ryall RD. The mesorectum in rectal cancer surgery—the clue to pelvic recurrence? Br J Surg 1982;69:613-6. [Crossref] [PubMed]
- Larsen SG, Pfeffer F, Kørner H, et al. Norwegian moratorium on transanal total mesorectal excision. Br J Surg 2019;106:1120-1. [Crossref] [PubMed]
- Wexner SD, Cohen SM. Port site metastases after laparoscopic colorectal surgery for cure of malignancy. Br J Surg 1995;82:295-8. [Crossref] [PubMed]
- Balli JE, Franklin M, Almeida J. How to prevent port-site metastases in laparoscopic colorectal surgery. Surg Endosc 2000;14:1034-6. [Crossref] [PubMed]
- Hol JC, van Oostendorp SE, Tuynman JB, et al. Long‐term oncological results after transanal total mesorectal excision for rectal carcinoma. Tech Coloproctol 2019;23:903-11. [Crossref] [PubMed]
- Atallah S, Sylla P, Wexner SD. Norway versus The Netherlands: will taTME stand the test of time? Tech Coloproctol 2019;23:803-6. [Crossref] [PubMed]
- Roodbeen SX, Spinelli A, Bemelman WA, et al. Local Recurrence After Transanal Total Mesorectal Excision for Rectal Cancer. Ann Surg 2020; [Epub ahead of print]. [Crossref] [PubMed]
- Deijen CL, Velthuis S, Tsai A, et al. COLOR III: a multicentre randomised clinical trial comparing transanal TME versus laparoscopic TME for mid and low rectal cancer. Surg Endosc 2016;30:3210-5. [Crossref] [PubMed]
Cite this article as: Lacy AM, Nogueira ST, de Lacy FB. Transanal total mesorectal excision into the future. Ann Laparosc Endosc Surg 2020;5:31.