Atypical and typical manifestations of the hiatal hernia
Introduction
Hiatal hernia is a common disorder characterized by protrusion of abdominal contents through the hiatus of the diaphragm and into the mediastinum. The condition usually involves the gastroesophageal junction (GEJ), but may include any abdominal structure. The extent of gastric and GEJ involvement, as well as herniation of additional abdominal organs through the hiatus, has evolved into the anatomical classification of hiatal hernias from types I through IV. In type I hernias, the GEJ migrates above the diaphragm into the mediastinum with the fundus and remaining stomach inferior to the GEJ. Type 1 hernias are referred to as sliding hiatal hernias and account for more than 95% of hiatal hernias (1). The remaining categories of hiatal hernias, types II though IV, are paraesophageal hernias. In type II hernias, the GEJ remains in the normal anatomical position with the fundus herniating cephalad though the hiatus. Type III hernias are a combination of types I and II and account for more than 90% of paraesophageal hernias (1). With type IV hiatal hernias, additional abdominal structures other than the stomach are herniated though the hiatus. The clinical manifestations of hiatal hernias vary and are impacted by the type and size of the hernia.
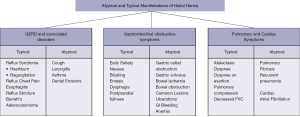
The true incidence and prevalence of hiatal hernia is difficult to quantify, as many patients remain asymptomatic and undiagnosed from the hernia. Of patients with symptoms, manifestations may be wide-ranging and include reflux, obstruction, pulmonary, and cardiac symptoms. Manifestations may be typical or atypical and comprise a broad differential that can make the diagnosis difficult for the clinician based on history alone. This article will review the typical and atypical manifestations of hiatal hernia. Manifestations of hiatal hernia will be divided into reflux and associated disorders, gastrointestinal obstructive symptoms and complications, and pulmonary and cardiac symptoms (Figure 1).
Gastroesophageal reflux disease (GERD)
GERD remains the most common presentation of a hiatal hernia. GERD is defined as a condition which develops when the reflux of stomach contents causes troublesome symptoms and/or complications (2). The prevalence of GERD in the United States (US) ranges from 18.1–27.8% (3) with a slightly lower 10–20% prevalence in Western Europe (3,4). The presence of a hiatal hernia is closely related to reflux symptoms and associated complications (5). Patients with a hiatal hernia are significantly more likely to present with GERD symptoms compared to those without a hiatal hernia (5). Furthermore, symptomatic GERD patients are more likely to have a hiatal hernia than those without symptoms (6,7). GERD symptoms are more common in Type 1 hiatal hernias, and the size of the hernia can impact symptom severity (5). GERD manifestations may be typical or atypical. Typical GERD symptoms are associated with esophageal syndromes with and without esophageal injury (2). Whereas, the atypical manifestations of GERD are more likely to involve extraesophageal syndromes.
Typical GERD symptoms manifest as troublesome heartburn and/or regurgitation (2). GERD is the most common cause of heartburn which is defined as a burning sensation in the retrosternal area (2). Weekly heartburn episodes are reported in 2–7% of patients with GERD (8,9), and episodes occur during sleep 25% of the time (10). In addition to heartburn, patients with GERD frequently present with regurgitation. Regurgitation is the perception of flow of refluxed gastric content into the mouth or hypopharynx (2). Together, heartburn and regurgitation can cause significant sleep disturbances and epigastric pain in patients with GERD. Surveys report a prevalence of sleep disturbance ranging from 23–81% in patients with heartburn and regurgitation (10-12). In addition, in two large randomized trials of acid suppression in reflux disease, 69% of patients presented with epigastric pain in addition to heartburn (13).
The symptoms of GERD can present with acute chest pain commonly referred to as reflux chest pain syndrome. The chest pain associated with GERD can be indistinguishable from ischemic cardiac pain and can occur without accompanying heartburn or regurgitation (2). In patients with hiatal hernias presenting with acute chest pain, acute coronary syndromes and acute aortic syndromes warrant initial investigation. Outside of these cardiovascular etiologies, GERD is the most common contributing factor for chest pain (14). Multiple studies have reported a population prevalence of chest pain of noncardiac origin up to 25% of patients (15-17).
The typical GERD syndromes of reflux and chest pain are not associated with esophageal mucosal injury on endoscopy. However, a number of typical esophageal syndromes with associated esophageal injury are common in patients with a hiatal hernia. These typical manifestations include reflux esophagitis, esophageal stricture, Barrett’s esophagus, and esophageal malignancy. Studies from the US and Western Europe have shown that 50–94% of patients with reflux esophagitis were diagnosed with hiatal hernia, whereas the prevalence of hiatal hernia was lower, 13–59%, in a control group (6,7,18,19). Esophageal strictures are present in <5% of patients with GERD and are characterized by persistent dysphagia (2). In patients with Barrett’s esophagus, the prevalence of hiatal hernia ranges from 72–96% (7,20). Additionally, studies have shown that the progression of Barrett’s to high grade dysplasia or adenocarcinoma was significantly and independently related to the presence and size of hiatal hernia (21,22). The associations between hiatal hernia and reflux symptoms, reflux esophagitis, stricture, Barrett’s esophagus, and esophageal malignancy are due to disruptions of different antireflux mechanisms and increased esophageal acid exposure resulting from a hiatal hernia (5). These impairments are beyond the scope of this review article and are presented elsewhere in this focused issue.
The strong association between hiatal hernia and GERD syndromes implies that many of the atypical presentations of GERD may manifest in a hiatal hernia. These atypical manifestations are often extraesophageal and rarely occur in isolation without concurrent typical symptoms of GERD. Atypical manifestations include chronic cough, chronic laryngitis, asthma, and dental erosions. Large population-based studies have demonstrated the increased risks of atypical symptoms in patients with reflux or esophagitis syndromes (15,23,24). Odds ratios (OR) range from 1.2–3.0 for having laryngeal or pulmonary conditions among GERD patients, with nocturnal cough having the strongest association (2). Dental erosions, commonly on the lingual and palatal tooth surfaces are more prevalent in patients with GERD (2). Patients presenting with atypical manifestations of GERD necessitate a broad workup as these symptoms are usually multifactorial with GERD as a potential aggravating factor.
Gastrointestinal obstructive manifestations
As previously discussed, hiatal hernias disrupt different antireflux mechanisms which lead to the strong association between hiatal hernia and typical and atypical manifestation of GERD. Furthermore, the mere presence of a hiatal hernia can produce a number of typical and, less commonly, atypical gastrointestinal symptoms and complications, unrelated to reflux. These symptoms result from the physical herniation of the stomach and additional abdominal structures through the hiatus. Hiatal hernias can disturb gastrointestinal filling, receptive relaxation, or continuity and produce various gastrointestinal obstructive symptoms.
Typical obstructive gastrointestinal symptoms of a hiatal hernia include early satiety, nausea, and bloating. These symptoms can be exacerbated with oral intake. Often patients complain of postprandial fullness in the chest or epigastrium which may limit oral nutrition and lead to subsequent weight loss. The pain is frequently described as a full or heavy feeling in the epigastrium and is relieved with emesis (25). Dysphagia and postprandial fullness occur as a result of esophageal compression by a progressively expanding herniating stomach (26). Hernia progression into the chest can also alter the angulation of the GEJ contributing to typical symptoms (26). As such, these symptoms are more frequently associated with paraesophageal hernias.
Atypical gastrointestinal obstructive manifestations of a hiatal hernia occur with less frequency. Progressive herniation of the stomach and additional abdominal structures can result in gastric outlet obstruction, gastric volvulus, or intestinal obstruction. Secondary gastric volvulus may arise from diaphragmatic defects, most commonly a paraesophageal hernia. Gastric volvulus associated with a paraesophageal hernia is most often organo-axial in orientation (27). Acute gastric volvulus can present as gastric strangulation resulting in acute, severe abdominal pain and retching, gastric necrosis, perforation, and sepsis. Alternatively, gastric volvulus can be intermittent or chronic leading to recurrent abdominal symptoms. Similarly, herniation of the small or large intestines in type IV paraesophageal hernias can present as bowel obstruction or intestinal ischemia with associated symptoms.
Other atypical manifestations of a hiatal hernia include gastrointestinal bleeding and anemia. The gastrointestinal bleeding associated with hiatal hernias can result from gastric ischemia in cases of strangulation or acute secondary gastric volvulus. Another etiology of gastric bleeding unique to hiatal hernias is ulcerations of the gastric mucosa known as Cameron lesions. These lesions present as linear ulcerations in the gastric mucosa in the fundus or body of the stomach. Proposed mechanisms for Cameron lesion formation consist of trauma secondary to diaphragmatic contraction on the herniated stomach, acid exposure, and local ischemia (28-30). Helicobacter pylori does not appear to play a significant role in the formation of Cameron lesions (30). The overall prevalence of Cameron lesions in a hiatal hernia is 3.3%, and increases as the hernia size increases (12.8% in hernias larger than 5 cm) (31).
The bleeding from Cameron lesions can present as an acute upper gastrointestinal hemorrhage in patients with a hiatal hernia. More frequently, the blood loss associated with hiatal hernia can be occult and present as iron deficiency anemia. The prevalence of Cameron lesions ranges from 1.9–9.2% in patients with iron deficiency anemia (32). However, iron deficiency anemia remains an atypical presentation of hiatal hernia in patients without Cameron lesions (33). Hiatal hernias increase the risk of iron deficiency anemia independent of esophagitis or ulcerations (34). The incidence of iron deficiency anemia in hiatal hernias is reported as 8–42% (35). In a study evaluating patients undergoing primary surgical repair of a hiatal hernia, anemia was present in 27% of the cohort and associated with increased postoperative complications (36).
Pulmonary and cardiac manifestations
Hiatal hernias can present with non-gastrointestinal symptoms, obscuring the diagnosis in such patients on initial presentation. As a hiatal hernia enlarges and more stomach or additional abdominal structures move into the mediastinum, respiratory manifestations may predominate (1). Typical pulmonary symptoms with hiatal hernia include dyspnea and atelectasis as a result of pulmonary compression. These patients may present with dyspnea on exertion or decreased exercise capacity as a result of reduction in forced vital capacity (37). Typical respiratory manifestations are more common with large paraesophageal hernias as compared to sliding hiatal hernias. Additionally, hiatal hernias are associated with such atypical pulmonary manifestations as pulmonary fibrosis.
The increased prevalence of GERD with hiatal hernias contribute to the association of a hiatal hernia with pulmonary fibrosis. In a study of more than 200,000 US Veterans, individuals with erosive esophagitis had a 1.36 OR of pulmonary fibrosis (23). In another study involving patients with idiopathic pulmonary fibrosis (IPF), the prevalence of a hiatal hernia and reflux was two times higher than in patient with a known cause of fibrosis (38). In a more recent study investigating the prevalence of a hiatal hernia on computed tomography (CT) in patients with pulmonary fibrosis, a hiatal hernia was present in 53% of patients with IPF (39). In this retrospective study, mortality from respiratory causes was significantly higher among IPF patients with a hiatal hernia than among those without a hiatal hernia (39).
As discussed previously, GERD associated with hiatal hernias may present as chest pain. Although this symptomatology is not cardiac in nature, hiatal hernias infrequently manifest as cardiac arrhythmias. In a large population-based study, hiatal hernias were associated with an increased prevalence of atrial fibrillation (40). In this study, hiatal hernia was associated with increased frequency of atrial fibrillation across all age groups, but particularly in younger patients with a 17.5-fold increase in men and 19-fold increase in women aged less than 55 compared to the general population (40).
Conclusions
Hiatal hernias may present in variety of ways, both typical and atypical. Manifestations are dependent on the type and size of the hernia. Gastrointestinal manifestations are the most common, predominately with GERD and associated syndromes. Typical GERD presents with heartburn and regurgitation as part of a reflux syndrome. Additionally, GERD may manifest as a typical chest pain syndrome unrelated to a cardiac etiology. Hiatal hernias associated GERD may present with esophageal mucosal injury in the form of reflux esophagitis, stricture, Barrett’s esophagus, and progress to esophageal malignancy. Atypical GERD symptoms like cough, laryngitis, asthma, and dental erosions may be may exist with hiatal hernias. GERD symptoms are more often associated with type 1 hiatal hernias.
Typical gastrointestinal obstructive symptoms of a hiatal hernia manifest as nausea, bloating, emesis, dysphagia, early satiety, and postprandial fullness and pain in the epigastrium and chest. Less common, atypical presentations include gastric outlet obstruction, secondary gastric volvulus, intestinal obstruction and ischemia, and bleeding. These manifestations occur more frequently with paraesophageal hernias. Bleeding, ulcerations in the form of Cameron lesions, and iron deficiency anemia are additional atypical manifestations of a hiatal hernia.
As hiatal hernias enlarge and move more into the thorax, non-gastrointestinal symptoms become more frequent. Typical pulmonary presentations consist of dyspnea, dyspnea on exertion, and atelectasis as a result of pulmonary compression. Similarly, compression on the left atrium may explain the higher prevalence of atrial fibrillation in patients with a hiatal hernia. Pulmonary fibrosis remains an atypical presentation of hiatal hernia, likely associated with the increased prevalence of GERD in a hiatal hernia.
Acknowledgments
Funding: None.
Footnote
Provenance and Peer Review: This article was commissioned by the Guest Editors (Lee L. Swanstrom and Steven G. Leeds) for the series “Hiatal Hernia” published in Annals of Laparoscopic and Endoscopic Surgery. The article has undergone external peer review.
Conflicts of Interest: All authors have completed the ICMJE uniform disclosure form (available at http://dx.doi.org/10.21037/ales-19-244). The series “Hiatal Hernia” was commissioned by the editorial office without any funding or sponsorship. The authors have no other conflicts of interest to declare.
Ethical Statement: The authors are accountable for all aspects of the work in ensuring that questions related to the accuracy or integrity of any part of the work are appropriately investigated and resolved.
Open Access Statement: This is an Open Access article distributed in accordance with the Creative Commons Attribution-NonCommercial-NoDerivs 4.0 International License (CC BY-NC-ND 4.0), which permits the non-commercial replication and distribution of the article with the strict proviso that no changes or edits are made and the original work is properly cited (including links to both the formal publication through the relevant DOI and the license). See: https://creativecommons.org/licenses/by-nc-nd/4.0/.
References
- Kohn GP, Price RR, DeMeester SR, et al. Guidelines for the management of hiatal hernia. Surg Endosc 2013;27:4409-28. [Crossref] [PubMed]
- Vakil N, van Zanten SV, Kahrilas P, et al. The Montreal definition and classification of gastroesophageal reflux disease: a global evidence-based consensus. Am J Gastroenterol 2006;101:1900-20; quiz 43. [Crossref] [PubMed]
- El-Serag HB, Sweet S, Winchester CC, et al. Update on the epidemiology of gastro-oesophageal reflux disease: a systematic review. Gut 2014;63:871-80. [Crossref] [PubMed]
- Stanghellini V. Relationship between upper gastrointestinal symptoms and lifestyle, psychosocial factors and comorbidity in the general population: results from the Domestic/International Gastroenterology Surveillance Study (DIGEST). Scand J Gastroenterol Suppl 1999;231:29-37. [PubMed]
- Hyun JJ, Bak YT. Clinical significance of hiatal hernia. Gut Liver 2011;5:267-77. [Crossref] [PubMed]
- Petersen H, Johannessen T, Sandvik AK, et al. Relationship between endoscopic hiatus hernia and gastroesophageal reflux symptoms. Scand J Gastroenterol 1991;26:921-6. [Crossref] [PubMed]
- Zagari RM, Fuccio L, Wallander MA, et al. Gastro-oesophageal reflux symptoms, oesophagitis and Barrett's oesophagus in the general population: the Loiano-Monghidoro study. Gut 2008;57:1354-9. [Crossref] [PubMed]
- Chen M, Xiong L, Chen H, et al. Prevalence, risk factors and impact of gastroesophageal reflux disease symptoms: a population-based study in South China. Scand J Gastroenterol 2005;40:759-67. [Crossref] [PubMed]
- Wong WM, Lai KC, Lam KF, et al. Prevalence, clinical spectrum and health care utilization of gastro-oesophageal reflux disease in a Chinese population: a population-based study. Aliment Pharmacol Ther 2003;18:595-604. [Crossref] [PubMed]
- Fass R, Quan SF, O'Connor GT, et al. Predictors of heartburn during sleep in a large prospective cohort study. Chest 2005;127:1658-66. [Crossref] [PubMed]
- Farup C, Kleinman L, Sloan S, et al. The impact of nocturnal symptoms associated with gastroesophageal reflux disease on health-related quality of life. Arch Intern Med 2001;161:45-52. [Crossref] [PubMed]
- Shaker R, Castell DO, Schoenfeld PS, et al. Nighttime heartburn is an under-appreciated clinical problem that impacts sleep and daytime function: the results of a Gallup survey conducted on behalf of the American Gastroenterological Association. Am J Gastroenterol 2003;98:1487-93. [Crossref] [PubMed]
- Vakil N. Epigastric pain in dyspepsia and reflux disease. Rev Gastroenterol Disord 2003;3:S16-21. [PubMed]
- Fass R, Achem SR. Noncardiac chest pain: epidemiology, natural course and pathogenesis. J Neurogastroenterol Motil 2011;17:110-23. [Crossref] [PubMed]
- Locke GR 3rd, Talley NJ, Fett SL, et al. Prevalence and clinical spectrum of gastroesophageal reflux: a population-based study in Olmsted County, Minnesota. Gastroenterology 1997;112:1448-56. [Crossref] [PubMed]
- Brattberg G, Parker MG, Thorslund M. A longitudinal study of pain: reported pain from middle age to old age. Clin J Pain 1997;13:144-9. [Crossref] [PubMed]
- Lampe FC, Whincup PH, Wannamethee SG, et al. Chest pain on questionnaire and prediction of major ischaemic heart disease events in men. Eur Heart J 1998;19:63-73. [Crossref] [PubMed]
- Kahrilas PJ, Kim HC, Pandolfino JE. Approaches to the diagnosis and grading of hiatal hernia. Best Pract Res Clin Gastroenterol 2008;22:601-16. [Crossref] [PubMed]
- Ronkainen J, Aro P, Storskrubb T, et al. High prevalence of gastroesophageal reflux symptoms and esophagitis with or without symptoms in the general adult Swedish population: a Kalixanda study report. Scand J Gastroenterol 2005;40:275-85. [Crossref] [PubMed]
- Cameron AJ. Barrett's esophagus: prevalence and size of hiatal hernia. Am J Gastroenterol 1999;94:2054-9. [Crossref] [PubMed]
- Weston AP, Badr AS, Hassanein RS. Prospective multivariate analysis of clinical, endoscopic, and histological factors predictive of the development of Barrett's multifocal high-grade dysplasia or adenocarcinoma. Am J Gastroenterol 1999;94:3413-9. [Crossref] [PubMed]
- Avidan B, Sonnenberg A, Schnell TG, et al. Hiatal hernia size, Barrett's length, and severity of acid reflux are all risk factors for esophageal adenocarcinoma. Am J Gastroenterol 2002;97:1930-6. [Crossref] [PubMed]
- el-Serag HB, Sonnenberg A. Comorbid occurrence of laryngeal or pulmonary disease with esophagitis in United States military veterans. Gastroenterology 1997;113:755-60. [Crossref] [PubMed]
- Gislason T, Janson C, Vermeire P, et al. Respiratory symptoms and nocturnal gastroesophageal reflux: a population-based study of young adults in three European countries. Chest 2002;121:158-63. [Crossref] [PubMed]
- Ellis FH Jr, Crozier RE, Shea JA. Paraesophageal hiatus hernia. Arch Surg 1986;121:416-20. [Crossref] [PubMed]
- Hunter JG, Smith CD, Branum GD, et al. Laparoscopic fundoplication failures: patterns of failure and response to fundoplication revision. Ann Surg 1999;230:595-604; discussion -6.
- Rashid F, Thangarajah T, Mulvey D, et al. A review article on gastric volvulus: a challenge to diagnosis and management. Int J Surg 2010;8:18-24. [Crossref] [PubMed]
- Cameron AJ, Higgins JA. Linear gastric erosion. A lesion associated with large diaphragmatic hernia and chronic blood loss anemia. Gastroenterology 1986;91:338-42. [Crossref] [PubMed]
- Moskovitz M, Fadden R, Min T, et al. Large hiatal hernias, anemia, and linear gastric erosion: studies of etiology and medical therapy. Am J Gastroenterol 1992;87:622-6. [PubMed]
- Weston AP. Hiatal hernia with cameron ulcers and erosions. Gastrointest Endosc Clin N Am 1996;6:671-9. [Crossref] [PubMed]
- Gray DM, Kushnir V, Kalra G, et al. Cameron lesions in patients with hiatal hernias: prevalence, presentation, and treatment outcome. Dis Esophagus 2015;28:448-52. [Crossref] [PubMed]
- Zullo A, Manta R, De Francesco V, et al. Cameron lesions: A still overlooked diagnosis. Case report and systematic review of literature. Clin Res Hepatol Gastroenterol 2018;42:604-9. [Crossref] [PubMed]
- Carrott PW, Markar SR, Hong J, et al. Iron-deficiency anemia is a common presenting issue with giant paraesophageal hernia and resolves following repair. J Gastrointest Surg 2013;17:858-62. [Crossref] [PubMed]
- Ruhl CE, Everhart JE. Relationship of iron-deficiency anemia with esophagitis and hiatal hernia: hospital findings from a prospective, population-based study. Am J Gastroenterol 2001;96:322-6. [Crossref] [PubMed]
- Panzuto F, Di Giulio E, Capurso G, et al. Large hiatal hernia in patients with iron deficiency anaemia: a prospective study on prevalence and treatment. Aliment Pharmacol Ther 2004;19:663-70. [Crossref] [PubMed]
- Chevrollier GS, Brown AM, Keith SW, et al. Preoperative anemia: a common finding that predicts worse outcomes in patients undergoing primary hiatal hernia repair. Surg Endosc 2019;33:535-42. [Crossref] [PubMed]
- Low DE, Simchuk EJ. Effect of paraesophageal hernia repair on pulmonary function. Ann Thorac Surg 2002;74:333-7; discussion 7. [Crossref] [PubMed]
- Mays EE, Dubois JJ, Hamilton GB. Pulmonary fibrosis associated with tracheobronchial aspiration. A study of the frequency of hiatal hernia and gastroesophageal reflux in interstitial pulmonary fibrosis of obscure etiology. Chest 1976;69:512-5. [Crossref] [PubMed]
- Tossier C, Dupin C, Plantier L, et al. Hiatal hernia on thoracic computed tomography in pulmonary fibrosis. Eur Respir J 2016;48:833-42. [Crossref] [PubMed]
- Roy RR, Sagar S, Bunch TJ, et al. Hiatal Hernia Is Associated With an Increased Prevalence of Atrial Fibrillation in Young Patients. J Atr Fibrillation 2013;6:894. [PubMed]
Cite this article as: Goodwin ML, Nishimura JM, D’Souza DM. Atypical and typical manifestations of the hiatal hernia. Ann Laparosc Endosc Surg 2021;6:39.